Seeing Clearly: Tips For Staining Cleared Tissue With Antibodies
Tips For Staining Cleared Tissue With Antibodies
By Ashley Juavinett
As early as 1914, there are documented attempts to try to “clarify” organ tissue, with the goal of enabling the study of these organs by removing light-scattering molecules. While many of those initial approaches are still being used today, researchers have recently returned to this century-old problem, with the hope of making the process compatible with modern techniques such as endogenous fluorescent proteins, in situ hybridization, and immunohistochemistry.
In 2013, Karl Deisseroth and his team made waves when they demonstrated advanced techniques to completely clear the brain, and by extension, other organs (Chung et al., 2013). Not only would this development save countless undergraduates from spending their summers in front of a microtome, but it also held promise of being able to visualize long-distance brain connectivity, with multiple rounds of immunostaining on the same tissue.
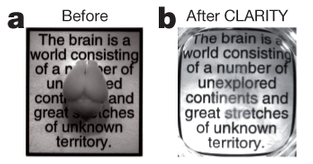
A demonstration of the powerful effect of CLARITY. From Chung et al., 2013.
Another method, known as PACT (“Passive Clarity Technique”), was subsequently published, and has since become a rival method for clearing brain tissue (Yang et al., 2014). In fact, many different methods have been published in the past five years, each with their own pros and cons (see table below). While some of these techniques are “active” - requiring electrophoresis or some other method to clear the tissue - most are “passive,” where the tissue is simply placed in multiple rounds of solutions to effectively remove the lipids.
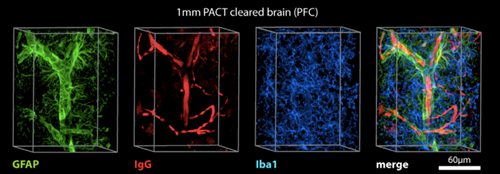
PACT clearing permits the labeling with a variety of common histological markers. From Yang et al., 2014
Table 1: A summary of recent optical clearing techniques:
(Links to publications can be found at the foot of the article.)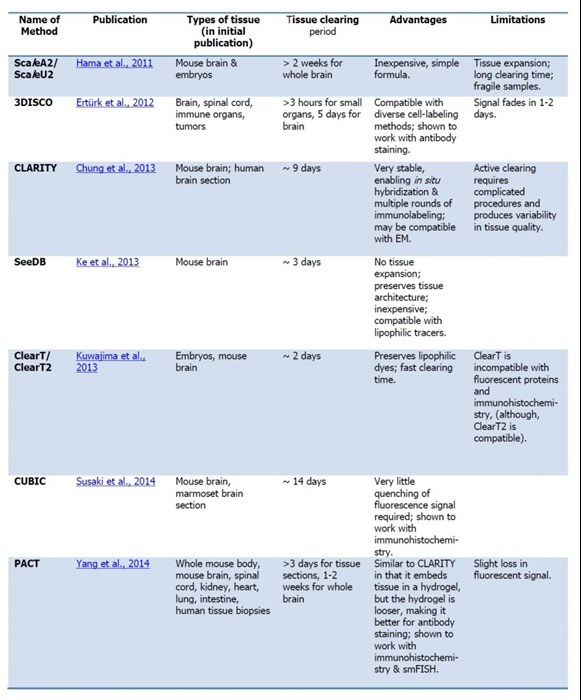
Cleared tissue staining tips
Since the development of these techniques, various labs have successfully immunostained cleared tissue, suggesting that this is indeed a viable method (e.g., Chung et al., 2013; Zhang et al., 2014). Still, not much has been said about the potential for multiple rounds of label beyond the initial CLARITY report. We spoke with several individuals* who have used these methods, and collected a few tips on how to make the best of your cleared immunostaining:
-
Immunostaining with cleared blocks of tissue takes longer than brain slices. According to the PACT protocol, it takes about 7-12 days for most immunostaining, depending on the type and size of tissue (more on that below). One study with CLARITY claims it can do it with 1 mm blocks of tissue in 1 day each for primary and secondary antibodies (Zhang et al., 2014, but keep in mind these are relatively thin tissue samples. The original paper says 2 weeks each for primary and secondary). However, keep in mind most studies are reporting the low end of the time, and generally, the more time, the better. For 2 mm chunks of brain tissue, our lab generally allows 2 weeks for staining.
-
Change the antibody solution as much as possible, perhaps more often than the given instructions. For a long incubation time, this will help decrease the amount of time necessary to label your tissue!
-
Use the smallest fragment possible (for secondary antibodies). For secondary antibodies, it works better to use Fab fragments rather than F(ab’)2 or whole IgG. The smaller the antibody (fragment), the better it can penetrate your tissue.
-
Trying using a denser antibody solution than you normally would for sliced tissue. Our lab recommends a 1:200 dilution for ~2 mm chunks of brain tissue, but you’ll need to experiment to see what works best for your sample. It’s always useful to run a titration experiment, with different dilutions but the same incubation time, to determine the optimal dilution for your experiment.
-
If you can, slice your tissue into smaller sections, no deeper than a few hundred microns. The less tissue your antibodies have to travel through, the better. If you can live with better staining on the periphery of the tissue, then you have less to worry about.
-
In our hands, the PACT method works better than CLARITY for immunostaining. Because the PACT matrix is a bit looser (it does not embed the tissue in a matrix hydrogel) there is more space for antibodies to penetrate. This means it will probably be more efficient to do immunostaining in conjunction with PACT. Our lab has yet to try immunostaining with other clearing methods.
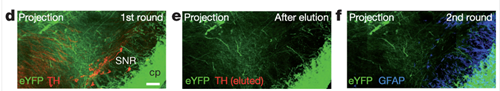
Chung and colleagues demonstrate multiple rounds of immunostaining (TH followed by GFAP) in the same brain tissue. From the initial Chung et al., 2013 report.
In general, the best thing to do is change the size of tissue, length of incubation, type of clearing, and concentration of antibody until you’ve achieved optimal labeling.
Do you have any experience with using clearing in conjunction with antibody labeling, particularly with Proteintech products? We’d love to hear about it!
* Thanks to Dr. Esther Richler & other members of the Callaway Lab for advice and insight!
References from Table 1
Hama et al., Nat Neurosci. 2011; 14(11):1481-8.
Ertürk et al., Nature Protocols 2012; 7(11):1983-95.
Chung et al., Nature 2013 16;497(7449):332-7.
Ke et al., Nature Neurosci. 2013; 16(8):1154-612013.
Kuwajima et al., Development 2013; 140(6):1364-8.
Susaki et al., Cell 2014, 24;157(3):726-39.
Yang et al., Cell 2014, 14;158(4):945-58.
Guest blogger profile
| Ashley Juavinett is a UCSD neurosciences PhD student, an NSF Graduate Research Fellow, and an aspiring science writer. Working at the Salk Institute (La Jolla, CA), Ashley is using in vivo imaging to investigate the neural circuitry underlying visual perception in mice. She currently co-directs a collaborative science writing group, NeuWrite San Diego (http://www.neuwriteSD.org), and writes about neuroscience and society on her own blog (http://scramblingforsignificance.blogspot.com). Follow her on Twitter: @ashleyjthinks |  |


